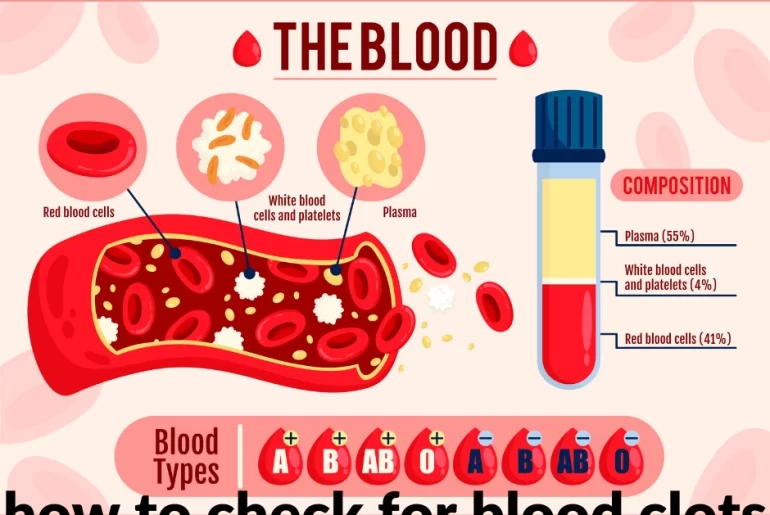
Blood clots, also known as thrombosis, can pose serious health risks if left undetected and untreated. They occur when blood for ms a gel-like clot within the blood vessels, disrupting the normal flow of blood. Blood clots can lead to various complications, including deep vein thrombosis (DVT) or even life-threatening conditions like pulmonary embolism. Therefore, it is crucial to be aware of the signs and symptoms of blood clots and know how to check for them. In this article, we will discuss the key methods for identifying blood clots and provide essential information on what to look out for to ensure prompt medical attention and appropriate treatment.
Table of Contents
Symptoms of blood clots
However, common signs and symptoms associated with blood clots include:
- Swelling
- Pain or tenderness
- Skin discoloration
- Warmth
- Redness
- Vein visibility
- Shortness of breath (in the case of pulmonary embolism)
Tests for blood clot diagnosis?
Tests for blood clot diagnosis may include:
Ultrasound: This non-invasive imaging test uses sound waves to create images of the blood vessels. It is commonly used to diagnose deep vein thrombosis (DVT) by identifying blood clots in the veins.
D-Dimer test: This blood test measures the levels of a substance called D-dimer, which is released when a blood clot breaks down. Elevated levels of D-dimer can indicate the presence of a blood clot, but further testing is usually needed to confirm the diagnosis.
Venography: This imaging test involves injecting a contrast dye into a vein and taking X-rays to visualize the flow of blood. It can help detect blood clots in the deep veins of the legs or arms.
CT scan or MRI: These imaging tests may be used to diagnose blood clots, especially in the lungs (pulmonary embolism) or other parts of the body. They provide detailed images that can help identify the location and extent of the clot.
Blood clotting tests: These tests measure the time it takes for blood to clot or evaluate specific clotting factors in the blood. They can help identify any underlying clotting disorders or abnormalities that may contribute to the formation of blood clots.
Risk factors for developing blood clots?
Several factors can increase the risk of developing blood clots. These risk factors can be categorised into three increase main groups:
Medical and Health Factors:
- Previous history of blood clots: Individuals who have had blood clots in the past are at a higher risk of developing them again.
- Certain medical conditions: Conditions such as cancer, heart disease, diabetes, and autoimmune disorders can increase the risk of blood clots.
- Surgery or hospitalization: Major surgeries, especially those involving the lower extremities or abdomen, and prolonged hospital stays can increase the risk of blood clots.
- Immobility: Prolonged periods of immobility, such as long-distance travel or extended bed rest, can promote blood clot formation.
- Hormonal factors: Pregnancy, childbirth, hormonal contraceptives (birth control pills, patches), and hormone replacement therapy (HRT) can increase the risk of blood clots.
Lifestyle and Behavioral Factors:
- Smoking: Smoking damages blood vessels and promotes clot formation.
- Obesity: Excess weight puts additional pressure on blood vessels and can disrupt normal blood flow.
- Sedentary lifestyle: Lack of physical activity and prolonged sitting or standing can contribute to blood clot formation.
- Poor diet: A diet high in saturated fats and low in fruits and vegetables can increase the risk of blood clots.
Genetic and Inherited Factors:
- Inherited clotting disorders: Certain genetic conditions, such as Factor V Leiden mutation or deficiencies in antithrombin, protein C, or protein S, can increase the risk of blood clots.
- Family history: Having a close family member with a history of blood clots can increase an individual’s risk.
Preventing blood clots
Preventing blood clots is crucial to reduce the risk of serious health complications. Here are some preventive measures that can help:
Stay active: Regular physical activity promotes healthy blood circulation. Engage in exercises such as walking, jogging, swimming, or cycling to keep your blood flowing and prevent clot formation.
Maintain a healthy weight: Obesity increases the risk of blood clots. Maintain a healthy body weight through a balanced diet and regular exercise.
Quit smoking: Smoking damages blood vessels and increases the risk of blood clots. Quitting smoking can significantly reduce this risk.
Stay hydrated: Drink an adequate amount of water to prevent dehydration, as it can contribute to blood thickening and clot formation. Stay hydrated especially during long flights or periods of immobility.
Take breaks during long periods of sitting or standing: If you have a sedentary job or need to sit for long periods, take breaks every hour or so to move around. Similarly, if you need to stand for extended periods, try to sit down and rest your legs whenever possible.
Practice leg exercises during travel: If you are on a long flight or car journey, regularly perform leg exercises such as ankle rotations, calf raises, and leg stretches to promote blood circulation.
Use compression stockings: Compression stockings apply gentle pressure to the legs, helping to prevent blood from pooling and reducing the risk of clots, especially during long periods of inactivity or when recovering from surgery.
Treatment options for blood clots
The treatment options for blood clots depend on the location, severity, and individual circumstances. The primary goals of treatment are to prevent the existing clot from growing larger, prevent new clots from forming, and reduce the risk of complications. Common treatment options include:
- Anticoagulant medications
These medications, also known as blood thinners, help prevent blood clots from forming and stop existing clots from growing larger. They do not dissolve the clot but allow the body’s natural processes to break it down over time. Examples of anticoagulant medications include heparin, warfarin, and direct oral anticoagulants (DOACs).
- Thrombolytic therapy
In some cases, when a blood clot poses an immediate and severe threat, thrombolytic therapy may be used. These medications, such as tissue plasminogen activator (tPA), are administered intravenously to dissolve the clot quickly.
- Inferior vena cava (IVC) filters
IVC filters are tiny devices placed in the inferior vena cava (the large vein that returns blood from the lower body to the heart) to catch blood clots and prevent them from reaching the lungs. They are typically used in cases where anticoagulant therapy is not suitable or effective.
- Compression stockings
Compression stockings can be used as a preventive measure for individuals at risk of blood clots or as part of the treatment plan. They help improve blood circulation in the legs and reduce the risk of clot formation.
- Catheter-directed thrombolysis
This minimally invasive procedure involves delivering clot-dissolving medications directly to the site of the clot using a catheter. It is commonly used for certain cases of deep vein thrombosis (DVT) or pulmonary embolism.
- Surgical intervention
In specific cases, surgery may be required to remove a blood clot. Procedures such as thrombectomy or embolectomy involve physically removing the clot from the affected blood vessel.
When to seek medical attention for a blood clot?
It is important to seek immediate medical attention if you suspect a blood clot or experience any of the following symptoms:
- Sudden onset of severe pain, swelling, or tenderness in the leg, arm, or other affected area.
- Unexplained swelling, warmth, or redness in the leg or arm.
- Chest pain or discomfort, especially if accompanied by difficulty breathing, rapid breathing, or coughing up blood.
- Sudden shortness of breath or difficulty breathing, even without chest pain.
- Coughing up blood or blood in your sputum.
- Rapid or irregular heartbeat.
- Dizziness, lightheadedness, or fainting.
- Sudden severe headache, slurred speech, confusion, or weakness on one side of the body, which could be signs of a stroke.
These symptoms may indicate the presence of a blood clot, especially if you have known risk factors or a history of blood clots. Prompt medical attention is crucial as blood clots can lead to serious complications, such as pulmonary embolism or stroke.
If you suspect a blood clot, it is important not to delay seeking medical help. Contact your healthcare provider, go to the emergency room, or call emergency services (such as 911 in the United States) to receive immediate evaluation and appropriate treatment.
FAQ
Q1: Can blood clots go away on their own?
Ans: Blood clots can sometimes dissolve on their own with the help of anticoagulant medications.
Q2: Are blood clots hereditary?
Ans: Certain clotting disorders can be inherited, increasing the risk of blood clots.
Q3: Can I prevent blood clots during long flights?
Ans: Yes, staying hydrated, moving around, and wearing compression stockings can help prevent blood clots during flights.
Q4: How long does it take to recover from a blood clot?
Ans: The recovery time varies depending on the location and severity of the clot, but it can take several weeks to months.
Q5: Can I exercise with a blood clot?
Ans: It is generally recommended to avoid vigorous exercise until the blood clot is properly treated and your healthcare provider gives approval.