Checking blood pressure is a crucial aspect of monitoring overall health and assessing cardiovascular well-being. Blood pressure refers to the force exerted by circulating blood against the walls of the arteries. High blood pressure, also known as hypertension, can lead to serious health complications if left uncontrolled. Conversely, low blood pressure, known as hypotension, can also have adverse effects on the body. Regularly measuring blood pressure allows individuals to detect any abnormalities and take appropriate measures to maintain optimal health. This article provides an overview of how to check blood pressure effectively, enabling individuals to take an active role in managing their cardiovascular health.
Table of Contents
What is considered normal blood pressure range?
The normal blood pressure range is an essential benchmark for assessing cardiovascular health. Blood pressure is typically measured using two numbers: systolic pressure and diastolic pressure. The systolic pressure represents the force exerted on the arterial walls when the heart contracts, while the diastolic pressure represents the pressure in the arteries when the heart is at rest between beats.
The standard unit of measurement for blood pressure is millimetres of mercury (mmHg). A normal blood pressure reading is generally considered to be around 120/80 mmHg. The systolic pressure should ideally be below 120 mmHg, and the diastolic pressure should be below 80 mmHg.
Here is a breakdown of the blood pressure categories:
Normal: Blood pressure below 120/80 mmHg.
Elevated: Systolic pressure ranging from 120-129 mmHg and diastolic pressure below 80 mmHg.
Hypertension Stage 1: Systolic pressure between 130-139 mmHg or diastolic pressure between 80-89 mmHg.
Hypertension Stage 2: Systolic pressure of 140 mmHg or higher, or diastolic pressure of 90 mmHg or higher.
Hypertensive Crisis: Systolic pressure exceeding 180 mmHg and/or diastolic pressure exceeding 120 mmHg. Immediate medical attention is necessary.
What are the symptoms of high blood pressure?
High blood pressure, also known as hypertension, is often referred to as a “silent killer” because it typically doesn’t cause noticeable symptoms in the early stages. However, as blood pressure levels rise significantly or remain consistently high, some individuals may experience certain symptoms or signs that can be attributed to hypertension. These symptoms may include:
- Headaches
- Shortness of breath
- Chest pain
- Fatigue or weakness
- Vision problems
- Irregular heartbeat
- Blood in urine
- Pounding in the chest, neck, or ears
- Dizziness or lightheadedness
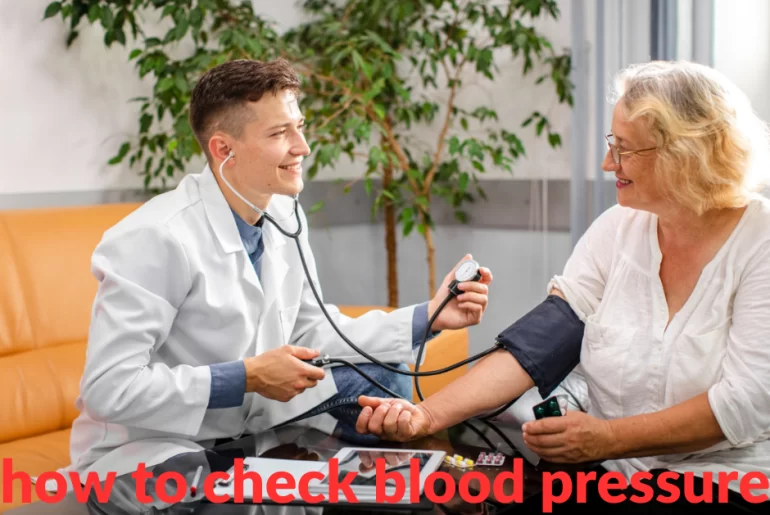
How to check blood pressure?
To check your blood pressure, you can follow these steps:
- Sit in a comfortable and relaxed position. Make sure you have been sitting quietly for at least 5 minutes before starting.
- Expose your upper arm, as it should be bare for an accurate reading.
- Wrap the blood pressure cuff around your upper arm. The lower edge of the cuff should be about 1 inch above the bend of your elbow.
- Position the cuff snugly but not too tight. It should be tight enough to stay in place but loose enough to fit one or two fingers between the cuff and your arm.
- Find a suitable place to rest your arm, such as a table or armrest, so that your arm is supported at heart level. The cuff should be at the same level as your heart.
- Locate the stethoscope or digital monitor display. If using a stethoscope, place the earpieces in your ears. If using a digital monitor, make sure it is properly set up and ready to use.
- Start the measurement. With a stethoscope, place the chest piece over the brachial artery just below the cliff’s edge. Inflate the cuff by squeezing the rubber bulb until it is snug around your arm.
- Slowly release the pressure in the cuff. If using a stethoscope, listen for the first thumping sound (systolic pressure) and the point where the thumping sound disappears (diastolic pressure). If using a digital monitor, it will automatically display the readings.
- Take note of the systolic and diastolic blood pressure values.
- Record the measurements, including the date and time, for future reference or to share with your healthcare provider.
How often should I check my blood pressure?
Here are some general guidelines:
- Healthy adults
If you have normal blood pressure (below 120/80 mmHg), it is advisable to check your blood pressure at least once every two years as part of routine healthcare visits.
- Prehypertension
If your blood pressure falls within the prehypertension range (systolic 120-139 mmHg or diastolic 80-89 mmHg), it is recommended to monitor your blood pressure more frequently, such as once a year, to identify any potential progression.
- Hypertension
If you have been diagnosed with hypertension or are on medication for high blood pressure, your healthcare provider will typically recommend more frequent blood pressure monitoring. This may include measuring your blood pressure at home and keeping a record to share during medical appointments.
- High-risk individuals
If you have certain risk factors for high blood pressure, such as a family history of hypertension, obesity, smoking, or underlying medical conditions, your healthcare provider may recommend more frequent blood pressure checks to closely monitor your cardiovascular health.
What are the risk factors for developing high blood pressure?
It is important to be aware of these factors to understand your own risk and take preventive measures. Here are some common risk factors associated with high blood pressure:
Age: Blood pressure tends to increase with age. The risk of developing hypertension rises significantly after the age of 40.
Family history: If you have a close family member (parent or sibling) with high blood pressure, you may have a higher risk of developing it yourself.
Obesity or overweight: Excess weight puts additional strain on the cardiovascular system and increases the risk of hypertension.
Unhealthy lifestyle: Poor dietary habits, high sodium intake, excessive alcohol consumption, smoking, and sedentary behaviour can all contribute to high blood pressure.
Lack of physical activity: Leading a sedentary lifestyle without regular exercise can increase the risk of developing hypertension.
Chronic conditions: Certain chronic conditions such as diabetes, kidney disease, and sleep apnea can contribute to high blood pressure.
Stress: Chronic stress and elevated levels of stress hormones can contribute to the development of hypertension.
Ethnicity: Some ethnic groups, such as African Americans, are at a higher risk of developing high blood pressure.
Gender: Men are generally at a higher risk of developing hypertension until women reach menopause, after which their risk becomes comparable to men.
Certain medications and substances: Certain medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs), oral contraceptives, and certain over-the-counter medications, as well as illegal drug use (e.g., cocaine), can contribute to high blood pressure.
FAQ
Q1: How often should I check my blood pressure?
Ans: Check it at least once every two years, or more frequently if advised by a healthcare professional.
Q2: What is considered normal blood pressure range?
Ans: Normal range is below 120/80 mmHg.
Q3: Can stress affect blood pressure levels?
Ans: Yes, chronic stress can contribute to high blood pressure.
Q4: What are the symptoms of high blood pressure?
Ans: Headaches, shortness of breath, chest pain, fatigue, vision problems, etc.
Q5: What are the risk factors for developing high blood pressure?
Ans: Age, family history, obesity, unhealthy lifestyle, chronic conditions, etc.